Retinopathy of Prematurity: What You Need to Know
Hello and welcome to Sight Research UK. If you're here, you're likely seeking answers about Retinopathy of Prematurity, perhaps for yourself or someone you care deeply about. We're here to help.
💌 Stay updated on ground-breaking sight research and new treatment developments by joining our mailing list.
What Exactly is Retinopathy of Prematurity?
Known as ROP, Retinopathy of Prematurity is a condition affecting the eyes of prematurely born infants. In this state, irregular blood vessels grow on the retina, the part of the eye that senses light and sends images to the brain. If not addressed timely, the condition can escalate to severe vision issues or even loss of sight.
Symptoms of Retinopathy of Prematurity
ROP often shows no immediate symptoms, making early diagnosis challenging. However, certain signs like crossed eyes, white pupils, or abnormal eye movements might be observed. Regular eye screenings are crucial for early detection.
What Occurs When a Child Has Retinopathy of Prematurity?
In ROP, blood vessels in the retina grow in an abnormal pattern, sometimes extending into the vitreous, the jelly-like substance inside the eye. This can cause scarring and even retinal detachment, putting the child's vision at risk.
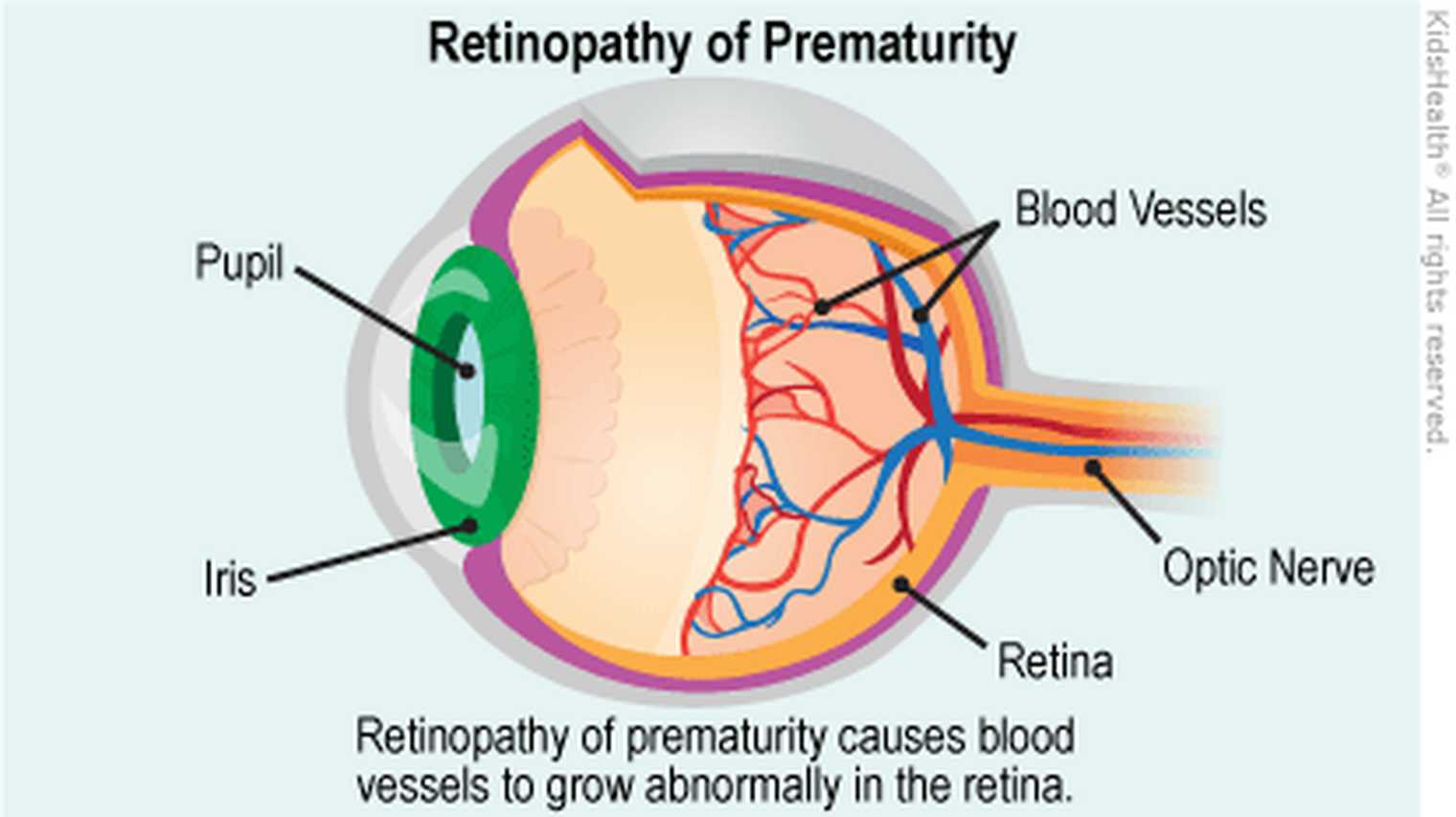
Kidshealth.org, 2022.
What Causes Retinopathy of Prematurity?
The exact causes of ROP are still under study, but premature birth remains a key factor. An undeveloped retina is more susceptible to irregular blood vessel growth. Oxygen therapy, often used in neonatal intensive care, is also a known contributing factor.
Can Retinopathy of Prematurity Be Treated?
Treatment strategies for ROP depend on the severity. Early diagnosis is essential for effective management. Treatment options include:
- Laser therapy
- Cryotherapy (freezing)
- Medication injections
Surgical Approaches: What Are They?
When ROP has advanced, surgical intervention might be necessary. The main surgical procedures are:
- Scleral buckle
- Vitrectomy
These surgeries aim to secure the retina in place, preventing further damage.
What Happens During a Retinopathy of Prematurity Surgery?
During the surgery, an ophthalmologist focuses on removing scar tissue and repositioning the retina. This can help avoid additional vision loss. Though not without risks, surgery is often the final option to preserve sight.
What Else Should You Look Out For With ROP?
Early intervention and regular check-ups are your best tools in effectively managing ROP. We're constantly funding research to learn more about this condition, and we're eager to share these advancements with you.
What Is The Current Status Of ROP Research?
We granted £69,748 to Dr Frank Proudlock, Associate Professor in Ophthalmology at the University of Leicester for a 3-year research project to speed-up and improve the diagnosis of ROP sparing thousands of premature babies from distressing, lengthy and unnecessary examinations. Click here to learn more about it.
Learn more about the life-changing eye research that we fund. Sign up to support a future free from sight loss.



